Wooley had a cerebral aneurism, a weak spot in a blood vessel that balloons out and fills with blood. About six million Americans -- 1 in 50 people -- have brain aneurisms that could rupture. Each year, aneurisms burst in about 25,000 people, and most die or suffer permanent disabilities, according to the Brain Aneurysm Foundation.
Dr. John Whapham, assistant professor in the Departments of Neurology and Neurological Surgery, Loyola University Chicago Stritch School of Medicine, used a less-invasive technique that's becoming increasingly common in brain surgery; he inserted a catheter (thin tube) in an artery in Wooley's leg and guided it up to her brain. The catheter released tiny platinum coils into the bulging aneurism, effectively sealing it off.
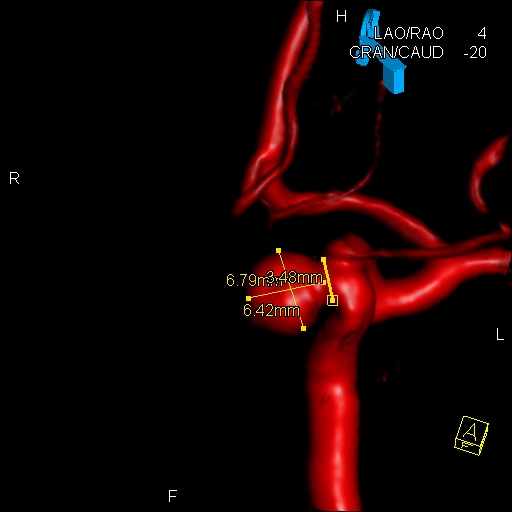
Norma Wooley's aneurism was 6.42 mm. across. Photo: Loyola University Health System
"She went home the next morning with a Band Aid on her leg," Whapham said.
Whapham, 36, is part of a new generation of neurologists who are using catheters to repair aneurisms, open clogged arteries, extract blood clots and repair blood vessel malformations in the brain. He also opens blocked carotid arteries in the neck. The catheter technique is much less invasive and risky than traditional brain surgery, which involves cutting a large opening in the skull.
Catheter technology, originally developed for heart surgery, has been modified for narrower and more challenging blood vessels in the brain. "There has been a huge evolution in devices over the last five years," Whapham said.
Whapham recently joined Loyola University Health System. He is board certified in neurology and has completed fellowships in endovascular neurosurgery, diagnostic cerebral angiography and stroke/neuro-critical care.
Wooley, 54, of St. Charles, Ill., is one of Whapham's first patients at Loyola. Her successful treatment illustrates the benefits of performing brain surgery with catheters rather than scalpels.
Wooley's aneurism was roughly one-fourth inch across, and shaped like a gumball. It could burst at any time and cause a debilitating or fatal stroke. Her clinical presentation was suspicious for what's called a "sentinel hemorrhage," in which an aneurism on the brink of rupture will often perforate without catastrophic clinical or radiographic findings. One day at work, Wooley began slurring her words, as if she had been drinking. Her mouth and eyelid drooped, and she had a headache that felt like someone was hitting her on the back of her head with a baseball bat. An ambulance took her to a local hospital, and she was transferred to Loyola.
"My brain was ready to explode," she said.
Traditional open-brain surgery to repair aneurisms is highly invasive, and recovery can take months. Many patients wind up with cognitive deficits that can, for example, make it impossible to do complex jobs.
Between 80 percent and 90 percent of brain aneurisms can be repaired with less-invasive catheters. Tiny coils of platinum wire are passed through the catheter and released into the bulging aneurysm. The aneurysm fills up with coils, causing the blood to clot. "It's like filling a bathtub with concrete," Whapham said.
A landmark clinical trial known as ISAT randomly assigned aneurism patients to receive either open brain surgery or catheter surgery. The catheter group had significantly lower rates of death and disability. Whapham said catheter surgery techniques and devices have improved dramatically since the study was published in 2002 in the British journal Lancet. "Technology is getting better by the week," he said.
"I put my life in his hands, and he gave it back to me," Wooley said of Whapham.






Comments