Plantar fasciitis is one of the most common causes of heel pain, affecting about 2 million people in the United States. It’s caused by inflammation of the plantar fascia, connective tissue that runs from the heel to the toes and supports the foot arch. The acute form of plantar fasciitis can be treated with stretching, shoe orthotics or cortisone injections. But about 10% of patients progress to the chronic form in which the foot’s collagen degenerates and the plantar fascia thickens. For these patients, surgical release of the plantar fascia with a small cut can help, but this surgery comes with risks, according to Beth Gusenoff, D.P.M., clinical assistant professor of plastic surgery at Pitt.
Inspired by the regenerative properties of fat stem cells, Gusenoff and husband Jeffrey Gusenoff, M.D., professor of plastic surgery at Pitt, developed a technique that uses fat harvested from a patient’s belly or other body area.
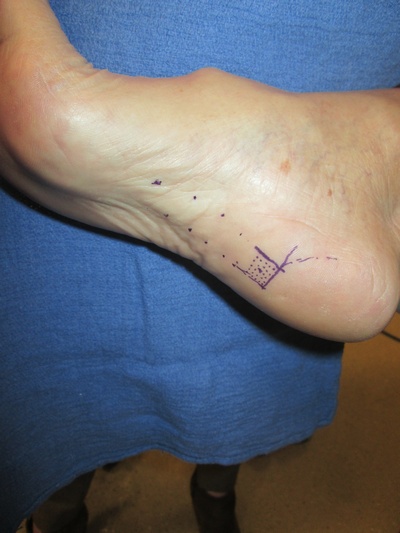
Credit: Gusenoff et al. 2022. Plast. Reconstr. Surg.
“In fat, there are stem cells and growth factors that help bring in fresh blood supply, which drives a mode of wound healing with reduced scarring,” explained Jeffrey Gusenoff. “We use a blunt needle to perforate the plantar fascia, which makes a small injury to stimulate the healing process. Then, when we pull the needle back, we inject a little bit of the patient’s fat.”
To test this method, the team recruited 14 patients with chronic PF and split them into two groups. Group 1 participants received the procedure at the beginning of the study and were followed for 12 months, and their Group 2 counterparts received the procedure after a six-month observation period and were followed for an additional six months.
“We found that Group 1 had improvements in quality of life and sports activity, decreased plantar fascia thickness and reduced pain levels,” said Jeffrey Gusenoff. “And a lot of the measures that were improving six months after the procedure got even better by 12 months.”
Similarly, Group 2 showed decreased plantar fascia thickness and increased sports activity six months after the procedure, and there was a slight, but not statistically significant, improvement in pain levels. With a larger sample size and a longer follow-up time, the researchers said it’s likely they would have seen stronger improvements in this group.
According to the Gusenoffs, this study provides proof-of-concept that fat injections can treat PF, and they now are planning a larger clinical trial to validate these findings. With enough evidence, they hope that the procedure will be deemed a medical necessity so that it can be covered by insurance and become more widely available in the future.






Comments