Obesity is associated with clear changes in gene-networks and the dysfunction of mitochondria, say researchers at the University of Helsinki and the National Public Health Institute - worse, the impacts of these cellular changes may aggravate and work to maintain the obese state in humans
Surprisingly, the genes most drastically affected by obesity were ones involved in the breakdown of a class of amino acids known as branched-chain amino acids. These changes in the obese twins were clearly associated with pre-diabetic changes in sugar metabolism and the action of the hormone insulin.
The researchers say that, while healthy eating habits and exercise are important, genes play some role in the development of obesity, so they studied rare cases of young (25 year old) identical twins with large differences in bodyweight and saw clear changes in the function of the cellular mitochondria.
“Identical twins share all the same genes and almost always are also identical in weight. Studying identical twins that do differ in weight is the best approach we have to get at the mechanisms involved in the interplay between genes and environment that result in obesity”, explains research scientist Kirsi Pietiläinen from the department of Public Health at the University of Helsinki, Finland.
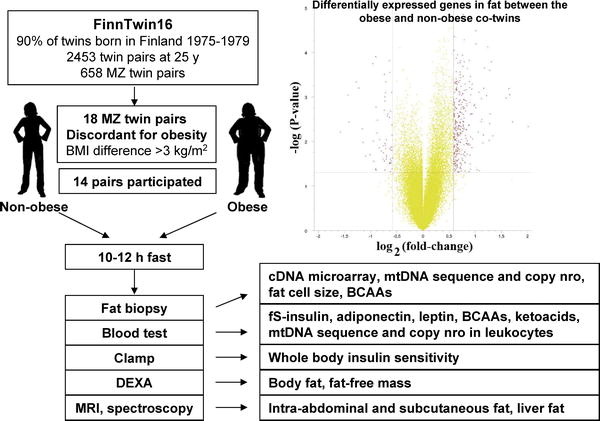
In a large collection of 650 pairs of Finnish twins born between the years 1975 and 1979, the researchers were able to identify only 18 pairs that at the age of 25 had developed more than a 10 kg (22 lb) difference in weight. The body composition and metabolism of 14 of these pairs was carefully studied and a sample of their fat was also obtained.
In a case where one of the identical twins is considerably heavier than the other, the reason behind this is not in the genes. Regardless of their identical genes, these genes can however be active at a different level. The research took advantage of this condition in order to characterize those changes in gene activity in fat tissue that result from obesity.
The researchers identified that the fat cells of the obese twins contained fewer copies of the DNA located in mitochondria. This DNA contains the instructions for energy use by the cell. “If one were to compare this cellular power plant with a car engine, it could be said that the engine of the fat individual is less efficient”, Pietiläinen says. An inefficient mitochondrial engine can also put out toxic exhaust. A clear sign of inflammation was observed in the obese twins’ fat tissue –a sign of the poor health of the cells.
Another sign of dysfunction in the mitochondria was also the much decreased breakdown of these branched-chain amino acids. What makes this observation especially important is the fact that the decreased breakdown of these amino acids, and their resultant increased concentration in the blood, was directly associated with pre-diabetic changes, fattening of the liver and the excessive release of insulin by the pancreas.
The research employed a gene-chip technology that enabled the scientists to measure the activity of all human genes. “By employing a genomewide method, biostatistics and the unique set-up of these identical twins, we were able to uncover new mechanisms behind obesity and the early diabetic changes in the metabolism of the fat twins.
In the future it will be important to determine whether these changes can be reversed by losing weight”, concludes Jussi Naukkarinen, a scientist at the department of Molecular Medicine, National Public Health Institute of Finland.
This study was supported by the US National Institute on Alcohol Abuse and Alcoholism (grants AA-08315, AA-00145 and AA-12502), the European Union Fifth Framework Program GenomEUtwin (http://www.genomeutwin.org/) (QLG2-CT-2002–01254), the Academy of Finland (Grant 44069, 100499 and 201461), the Academy of Finland Centre of Excellence in Complex Disease Genetics and in Mitochondrial Disease and Aging (FinMIT), the Nordic Center of Excellence in Disease Genetics, Sigrid Juselius Foundation, Biocentrum Helsinki Foundation and Helsinki University Central Hospital grants. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Article: Pietiläinen KH, Naukkarinen J, Rissanen A, Saharinen J, Ellonen P, et al. (2008) Global Transcript Profiles of Fat in Monozygotic Twins Discordant for BMI: Pathways behind Acquired Obesity . PLoS Med 5(3): e51 doi:10.1371/journal.pmed.0050051






Comments